Introduction
In New York alone, every six hours, someone dies of a substance use overdose. That’s unbelievable, every six hours. Like others before me, I’ve had the sad and deeply troubling experience of being witness to a human being dying on the streets of New York City from a drug overdose. This was a tragedy that could and should have been prevented.
Confronting the raging opioid pandemic is the first step to understanding the varied complexities. Over the years, substance abuse has had a major impact on people’s lives across the U.S. As alarming as it may sound, the fact remains that opioid-related drug overdoses take the lives of more than 130 people a day. The ripple effect of the opioid crisis extends far beyond the traditional primary care system.
Substance abuse issues, and speaking about this around the world, is one of the areas of my expertise, particularly as part of an overall integrated healthcare process–a process that combines primary care, mental health and substance use clinics.
The role of primary care providers can make all the difference in SUD (substance use disorders); the best approach is to integrate early substance disorders prevention services and offer a more effective and safe pain management plan. Similarly, primary care providers should roll out the MAT (medication-assisted treatment) program into the integrated healthcare services. More integrated healthcare services can include promoting telemedicine services, offering technical assistance, building a robust healthcare workforce, and expanding existing integrated healthcare service models.
The Grim Reality of Opioid Crisis
Young individuals who don’t have a supportive family, safe housing, job prospects, and a decent education are the real victims of the opioid epidemic. In fact, the data continues to paint an even more startling picture of substance abuse amidst the coronavirus outbreak.
Many young people are exposed to illicit drugs due to homeless and isolated conditions. The underbelly street life has always been here, but the numbness that stems from drug use creates more loss of life for local communities and families.
The opioid epidemic is not limited to homelessness. Opioid abuse is a tragedy that is impacting individuals with different socio-economic spectrums. However, social dynamics and capital that involve employment opportunities, housing, educational reforms, spiritual coaching, mentoring, family support, childcare, and vocational training help people remain clean.
Unfortunately, the current state of opioid abuse is spreading like wildfire in the U.S. It would be fair to say that the time to create an aggressive and realistic public health response has become the need of the hour for America.

Substance Abuse and COVID-19 Susceptibility
As the coronavirus pandemic crisis spirals out of control, the opioid and substance abuse individuals have become more vulnerable than ever. The cat is out of the bag, and it is no secret that the COVID-19 outbreak is putting the lives of people with opioid use disorder in grave danger.
Practically, these marginalized and vulnerable individuals heavily rely on in-person healthcare services. But prolonged lockdowns and social distancing measures continue to create more treatment challenges. With the COVID-19 pandemic crisis, alcohol relapses have become more common in the U.S. In fact, a recent study concluded that individuals with substance use disorders are far more vulnerable to COVID-19-related complications.
Substance Abuse: Focus on the Key Facts and Figures
According to the National Center for Drug Abuse Statistics (NCDAS):
- In the U.S., there have been more than 700,000 drug overdose deaths since 2000.
- In 2018, almost 20% of the American population had exposure to illicit drugs.
- In 2018, almost 12% of the American population over 12 years old was using illegal drugs.
- In 2018, almost 20% of the American population, 12 years or older, had misused prescription drugs. In the same year, there was increased usage of heroin, cocaine, marijuana, prescription stimulants, methamphetamines, prescription pain medication, and prescription sedatives.
- As of now, the most abused form of the classified drug is marijuana with over 4.4 million people.
- The mixture of tobacco and alcohol became more detrimental to the health of the addicts. In fact, American substance users rose to 165 million just two years ago.
- In 2019, the poison control center managed to handle more than 5231 e-cigarettes, vaping, and liquid nicotine cases in the U.S. In 2020 alone, however, there are already up to 1203 cases.
- In 2019, more than 20 million individuals aged 12 or older had reported substance abuse.
- Almost 15 million Americans have an alcohol abuse disorder.
- Comparatively, metropolitan citizens report more than 20% use of illegal drugs while people who reside in rural counties and non-metropolitan areas report just 5%.
- Over 2 million Americans have had an opioid disorder such as heroin abuse or prescription pain reliever.
There’s More than One Type of Drug
Narcotics are the most abused drug that involves opium and opium derivatives. Similarly, stimulant abuse transpires in illegal and legal forms. Common prescription stimulants are Dexedrine, Adderall, Ritalin, Modafinil, etc.
‘Bath salts’ on the other hand, refer to street drugs like cocaine, methcathinone, methamphetamine, and various synthetic cathinones. Alternatively, synthetic hallucinogens come from fungi and plants. It is vital to note that most hallucinogens do not equate to medical treatment and have illegal status in the U.S.
‘Crossfade’ refers to the combination of alcohol and marijuana that increases the absorption of THC and alcohol impairment. In terms of addiction patterns, it is hard to overlook the overdependence factors and mental health issues.
Over time, drug use creates a psychological and physical dependence such that more awareness is needed; non-medical, non-prescribed, and non-sanctioned use of controlled substances falls under drug abuse.
Spike in Drug Overdose Death Rates
Contemporarily, there is no government-sanctioned track-and-follow system for drug users in the U.S. Fortunately, the NCHS at the CDC does, in fact, collect data on the most commonly abused drugs.
More than 65,000 Americans died from a drug overdose that involves prescription opioids and illicit drugs in 2019. Between 2010 and 2017, the total number of drug overdose deaths jumped from 38,329 to 70,237.
Drug Overdose Deaths in America (1999-2018)
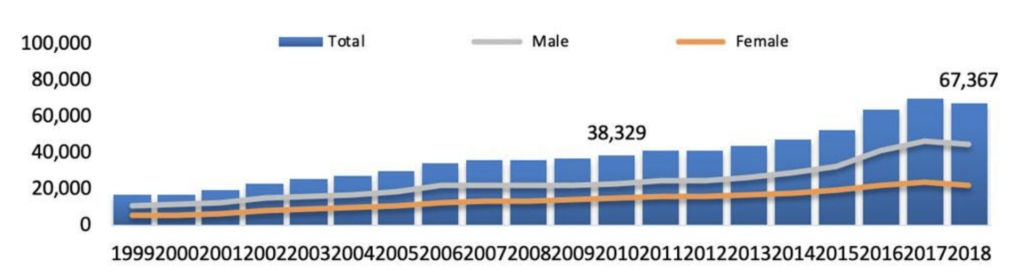
Although in 2018 the drug overdose saw a decline, there were more reported deaths from synthetic narcotics. The usual suspects include psychostimulants or cocaine with high abuse potential in the upward direction.
Drug Overdose Death in America (Illegal and Prescription Drugs)
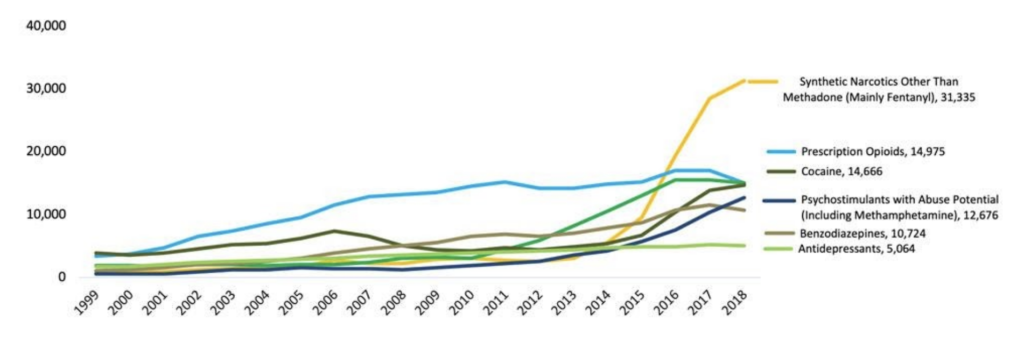

Opioid Use and Disorder: How Integrated Care Comes into the Picture
CDC research highlights that one out of four patients who get primary long-term opioid therapy struggle with their opioid use disorder. The curse of opioid addiction is now affecting the way physicians prescribe medication.
Nonetheless, the medical community understands the need for more treatments to make the recovery process faster for opioid addicts under treatment. Primary care providers can make the most out of an integrated approach throughout the opioid recovery process.
Recent research pinpoints the significance of a holistic approach to ensure opioid recovery in a modern community setting; it is realistic to base group counseling, individual counseling, medication management, relapse prevention medications, psychiatric treatment, and mental health therapy as a program model.
Before implementing an integrated care approach, primary health providers have to address various stigmas related to drug use treatments. However, limited mental health resources, access to holistic treatment options, navigational challenges, and access to specialized healthcare providers are some of the problems associated with substance abuse treatment.
If primary healthcare providers want to adopt a successful integrated approach, there will have to be efforts to make patients more comfortable and safe for a full recovery. While there are many facets of an integrated approach that ensures successful treatment and recovery for patients, primary healthcare providers should focus on the key tactics.
Merging Medication-Assisted Treatment (MAT) with Psychosocial Interventions
Psychosocial interventions are necessary because they do more than just save lives; they assist patients to learn more skills and understand social dynamics required to achieve long-term recovery. Besides, psychosocial interventions can help primary providers realize the healthcare needs of individuals suffering from opioid abuse.
Once you can identify specific conditions that likely led to the abuse, it would become easier to help patients recover better. Contrary to misguided perception, it is not a new phenomenon. In fact, one research proves that substance abuse patients who undergo MAT and psychosocial interventions have a better chance of recovery than others do.
Mixed or Virtual Treatment Approach
Even with limited resources, primary healthcare providers can offer opioid recovery support. The answer lies in the amalgamation of in-office and virtual services that can create a foundation for an integrated approach. You can look at the same integrated approach through telehealth services.
For instance, telehealth case supervisors can become the primary contact for the addict during the recovery process. Case supervisors can help medical staff and physicians detect early warning symptoms of opioid addiction and possible relapse.
Furthermore, telehealth counselors can determine the behavioral and mental health requirements for difficult patients. Similarly, certified recovery specialists can also play a crucial role and encourage, connect, and coach through relevant community resources.
Physical Problems and Addiction: Connect the Dots
It is true – one or more physical problems can make the addiction worse. In fact, an extensive survey draws healthcare providers’ attention that pain relief is the main reason that drives most people to misuse opioids.
Once you understand the cause-and-effect relationship between physical problems and addiction, it becomes clear to implement a team-oriented and integrated approach for opioid treatment and recovery.
Pain management experts can also find alternative medications for patients suffering from severe opioid addiction. Through motivation interviews and digital therapy, opioid addicts can recover faster and explore healthy living options.
For instance, people who suffer from chronic physical pain need to have a consistent exercise routine. Patients can coordinate with a pain specialist or physical therapist to determine a useful exercise for recurring pain. In fact, cognitive-based therapy often garners the same results as pain medications.
Involvement of Family Members Matters
Patients throughout the opioid treatment and recovery process can benefit from the continuous support from their family. Emotionally, close family members can reinforce values that would encourage the patients to recover faster.
However, in many cases, family issues contribute to substance abuse. Therefore, it is a subjective element that requires individual research. In essence, you’d be surprised how each patient’s relationships and habits can leave an impact on the overall treatment and recovery process.
Confront and Resolve Common Stigmas
It is the age of scientific, IT, and the digital revolution, but many patients still avoid opioid addiction treatment because of societal and environmental stigmas. Again, the best way to thwart most stigmas is through combined MAT and psychosocial intervention treatment.
Scientifically, MAT reduces the opioid cravings and leads to withdrawal. It has become one of the most effective treatments for opioid addiction. Often, the stigma comes down to MAT, and that includes medical professionals.
Physicians profess that many patients who have opioid addiction show their grievances about lack of staff, space, care management, and mental support. Eventually, these factors become major obstacles in MAT treatment. Therefore, it makes sense to confront stigmas associated with the practical use of MAT to ensure a successful recovery.
Health leaders can offer MAT education to addiction professionals, family members, and physicians to improve the recovery chances of patients. In time, it will also clear the fog of stigmas among patients. Ordinarily, primary healthcare providers can introduce lunch-and-learn training sessions for medical staff, nurses, and physicians.
Substance Abuse and Opioid Crisis: What Lies in the Future?
More primary healthcare providers need to understand that substance abuse stems from a variety of destructive family and social conditions. It could be academic failures, family conflicts, domestic violence, crime, financial issues, child abuse, or lost productivity. Once you establish root parameters, you can fill in a lot of blanks.
The current estimates suggest that the collective cost of substance abuse will exceed an annual $600 billion in the U.S. However, prompt integration of mental health services into a primary care setting creates a win-win situation for patients and healthcare providers. The integrated model can include various substance abuse disorder services. An integrated care model can significantly increase communication, coordination, and access for individuals with opioid use disorders.
As a board member of both Treatment Communities of America (TCA) and the World Federation of Treatment Communities (WFTC), and as a United Nations representative for the World Treatment Federation of Substance Users, one of the things that I’ve always had to look at, first and foremost, was the integrated care model at organizations and the need for mental health access for substance users. Another area of address was the type of communications between ambulatory care/primary care physicians and their patients who are suspected of having substance use issues; there is a need to ask the right questions and a need for training our mental health and primary care physicians on how to deal with potential substance use patients.

PDV Health Consulting: The Next Stage of Integrated Care Solutions
Since the beginning, PDV Health Consulting has understood the vitality of addressing mental health issues among people suffering from opioid addiction. The last thing a primary care provider should do is confuse a substance use counselor with a mental health counselor. Our evaluation criteria depend on whether or not a particular patient required medication.
Through an integrated care model, primary care providers can address mental health issues and understand the background of substance abusers. Our years of experience have taught us that trust bridges the gap between the patient and the doctor. However, to build long-term trust, primary care providers need to create a certain degree of awareness without judging the patients.
In retrospect, patients need more than just medication; they need mental health support to recover from addiction. We champion those hundreds and thousands of NA meetings that patients share with their counselors. At PDV Health Counseling, we believe that the act of sharing what patients experience and go through can open new windows of opportunities to speed up the recovery process.
Conclusion
The need for a more supportive and successful healthcare solution to battle the current opioid epidemic has never been more relevant. In fact, there has to be an integrated approach that considers the health requirements of people suffering from severe substance addiction. No extensive integrated treatment method means patients will have to face more hurdles to transition from opioid addiction.
Technological advancements and behavioral segmentation can help primary healthcare providers create an integrated approach that would pave the way for faster opioid recovery and ensure successful treatment. In hindsight, the secret lies in empowering more patients to beat their addiction and live healthy and prosperous lives.

