It’s an obvious understatement to say how much the world has changed since the COVID-19 pandemic began. According to the latest data provided by The Johns Hopkins Coronavirus Resource Center (CRC), the coronavirus continues to inflict its damage around the world with cases rising in various regions. At the time of this writing, there have been well over 30.2 million cases and 947k deaths globally. Of that, there were over 6.6 million cases and 197,946 deaths in the US alone. In New York, my home town, over 33 thousand lives were lost–all these numbers are tragically staggering to humanity.
Another understatement can be made as relates solely to this article: that the pandemic has also taken a heavy toll financially on healthcare facilities across the US. It has put many hospitals, nursing homes, ambulatory care, and home care companies in budgeting challenges, and not only from changes in the payer mix, but from the costs that were associated with COVID. Even though many states received federal COVID funding, health organizations still find themselves unable to determine how to budget for their next fiscal year. In fact, just the ambulatory care organizations alone, many have lost almost 80% of their business and are just starting to recover some of that now.
That said, what budgeting strategies can healthcare organizations implement to continue operating with quality, success and sustainability?
First we need to understand how healthcare costs and utilization amidst the COVID-19 pandemic has changed. As the world grappled with the new crisis, many hospitals decided to cancel elective medical procedures to cut back on costs.
Despite careful planning, hospitals continued to incur the curse of added costs. Realistically, the coronavirus cases will mount to more costs than previous calculations. In fact, the average case would require more medical supplies and labor for the continuation of treatment.
Fortunately, healthcare leaders are diverting their attention to understand the long-term impact rather than solely focus on short-term consequences throughout the COVID-19 crisis. However, the financial ramifications will be unique for each sector and even individual organizations.
Let’s take a look at the analytical factors and budgeting strategies that healthcare organizations need to pay more attention to, during and after the COVID-19 pandemic:
Healthcare Standards: The Capitalist Order is Changing
Humans no longer have to absorb the mountainous accumulated data. Whether it’s technological advancements or digitalization, the processing of operations has never been easier for healthcare organizations. Still, the market is on edge due to the continued threat of the coronavirus pandemic.
In fact, it is one of the reasons more healthcare organizations are focusing on results-oriented long-term measures and objectives to thwart financial difficulties in the foreseeable future. More organized budget and cost control initiatives will help hospitals monitor the budgeting cycle and implement informed management solutions.
Today, any healthcare organization’s executive staff needs to review and maintain positive cash-flow in times of dire financial circumstances. Regular flash reports should become the norm for healthcare organizations in case of any surge in COVID-19 cases and would also paint the picture of the pandemic crisis to the board of directors. The solution lies in reviewing the intricate details of your budget.
From admissions to COVID-19 cases to case index to cash-flow, organizations need to keep an eye on all essential budgeting components. The higher the focus on regular monitoring, the more informed you can be about the potential budget constraints. Ideally, you need to ensure that sufficient resources are in place to get relevant PPE or other equipment.
COVID-19 and Financial Challenges for Health Organizations
Currently, researchers predict that 90% of healthcare organizations that have decided to halt elective procedures would start to see negative profit margins throughout the COVID-19 period. As harsh as the data may sound, healthcare financial experts need to be more skilled to understand the complex details associated with costs.
In fact, the understanding of a financial model should be the basis on which to make informed decisions for current and future operational processes.
What Makes Budgeting an Essential Component of a Perfect Strategic Plan?
Budgeting is a detailed and pre-planned process of devising a plan that focuses on how you will spend your money. Once you devise a spending plan, it will enable you to establish whether or not you will have sufficient money to undertake various operations beforehand.
Unlike traditional short-term budgeting, strategic budgeting revolves around devising a long-term budget plan that can last for more than a single year. The need of the hour dictates a strategic budget plan that can help healthcare organizations fulfill their vision and retain position in the industry.
The planning process becomes essential when you don’t have enough means and resources to prioritize numerous operations. Following a long-term strategic budget plan is a perfect way to resolve current debts and remain debt-free. A long-term budget is crucial in allowing healthcare organizations to be more realistic and forecast entire spending prior to annual financial planning. As a result, you would not have to make presumptuous financial mistakes and plan for long-term budget goals.
Additionally, the endless hospitalizations are a crucial metric for healthcare organizations to estimate the COVID-19 toll and their ability to handle the situation.
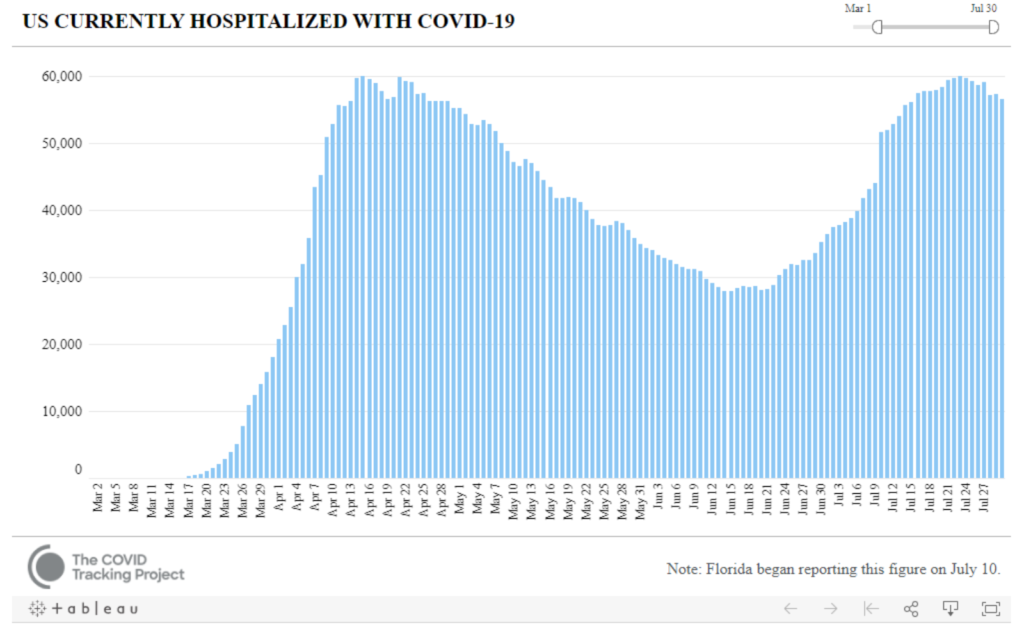
US Coronavirus Hospitalization Chart for the Month of July
Best Budget Strategies: From Continuous Monitoring of Revenue Cycle to Cash Flow Mitigation
Currently, only 57% of medical centers and hospitals have an efficient cost accounting system. In fact, most healthcare organizations don’t have a digitalized modern system to analyze data and decrease patient care costs.
Reduce Cash Flow Problems
Prioritize Your Money First
Your first course of action should be to prioritize how you intend to spend cash in the future. After that, you can evaluate the list of accounts payable to find out the vendors that are valuable at the moment. The trick is to make a comparative analysis and focus on elements that matter the most at the moment.
Get Vendors’ Confidence
Another way you can reduce your cash flow issues is to always keep the company of essential vendors. In fact, there’s a good chance you will need the help of reliable vendors to get through the nightmare of low or negative cash flow.
Remember, most suppliers are huge firms that have the freedom to be financially flexible with regular customers. So long as you build a positive relationship with vendors, they will be open to bridge gaps and work with you during a crisis.
Seek Help from Your Insurance Representative
Insurance representatives can offer you the coverage you need to be more flexible and manage your cash flow. For the most part, insurance companies have short-term flexibility to grant reductions or interruption in the premium.
For instance, if your healthcare organization has interruption insurance coverage, it can safeguard you against current and future losses that stem from COVID-19 or natural causes. Therefore, get in touch with your insurer to extend your coverage to mitigate COVID-19 losses. Later on, you can file a claim to document all your business losses.

Keep an Eye on Your Revenue Cycle
When it comes to revenue cycle, you can outsource to third parties or implement an effective RCM software. As a result, you would be able to authorize patients before each service, submit claims, deal with payments, generate reports, manage denials, and establish eligibility of patients.
Technically, the revenue cycle refers to financial processes, management of funds, and collection of payments that result from patient care. In essence, every organization needs a revenue cycle process to ensure an errorless billing cycle.
Outsourcing
The revenue cycle starts with how you outsource your operational processes. Typically, it depends on the size of your healthcare organization that determines the overall operations. Fortunately, medical firms don’t have to be well-versed in technical details. Instead, employ an efficient IT team that can take care of the medical billing through a dedicated revenue cycle management solution.
Pre-Authorization
Another component of your revenue cycle should focus on the pre-authorization of all patients. Pre-authorization refers to a definitive decision that a health plan or insurer takes to deem the necessity of a medical procedure, equipment, or prescription medication. The only exception in the pre-authorization of a patient occurs in emergency cases.
It is vital to remember that pre-authorization does not equate to coverage of cost by your insurer. It means healthcare providers and patients double-check the coverage if there’s any doubt.
Submission of Claims
Evidently, you can’t expect payments to finalize until you submit claims for the services rendered to different patients. Healthcare organizations can, for instance, deploy practice management practices to keep up with the billing processes.
On the other hand, you can use practice management software to automatically submit claims. As a result, you would be able to submit claims in batches. Realistically, your claim submissions are bound to run into a human error. It is a factor that healthcare organizations have to contend throughout the submission of claims. An automated claims management solution would be a better choice to detect mistakes and make recommended fixes. Subsequently, you can resubmit a patient’s claim immediately. The more control you have over your claims, the more common errors you can eliminate.
Reporting
According to a recent Deloitte report, “COVID-19 should be taken into consideration when preparing the annual report”
That said, your healthcare organization cannot afford to deal with hidden problems that get worse over time. Mostly, these hidden issues stem from the non-availability or preparation of detailed reports. Therefore, your medical practice should produce a wide array of reports that serve specific purposes.
It is, of course, a perfect way to keep the board of directors and management in the loop about the financial situation. You can, for instance, generate customized reports through a revenue cycle management solution.
The idea is to get a complete overview of your financial data, main performance indicators (KPI’s), and management information. Furthermore, a modern revenue cycle management solution can simplify the processes that would make your medical staff more productive.
Mass Registration
You can register patients by cross-training your coding staff and billing processes. Your underlying objective should be to strengthen your revenue cycle. Besides, coders and billers are aware of the fact that registration can resolve problems during a financial crisis.
Gone are the days of conventional access points. Today, you can get rid of bottlenecks and take care of high demand registration access points that would speed up the treatment process. Develop a detailed registration process through modern technological devices–an all-in-one that’s ready to register on a laptop or mobile device is a win-win for patients and healthcare organizations.

Expect the Unexpected: Why It Makes Sense to Prepare for the Worse
Although all components of a strategic plan matter, the budget is arguably the most relevant one. It takes a certain degree of creativity, planning, and timing to take care of budgeting. There’s no such thing as small budget changes. In fact, healthcare organizations have to discuss and get the board of directors’ confidence before implementing a medical protocol.
Despite the nature of a challenge, it should result in a solution. It may sound straightforward at first, but you will have to assume different budget scenarios to come up with viable solutions.
And the center of attention throughout discussions should be preparedness of worse-case budget setup. Think of it as a contingency plan that would help you get through a spike in COVID-19 cases and take care of minute-to-minute in-house operations.
For instance, if you might need capital equipment in the coming months, figure out how you would deal with it beforehand. Essentially, you need to focus on a controlled revenue cycle. It should be able to explain the worse-case budget scenarios and possible solutions to sustain positive cash flow. Just like cash-flow consideration, you will also have to take into account temporary payroll redundancies in your budget. It is a matter that requires the utmost due-diligence to inform the Board members.
The Need for More Transparency and Communication
Transparency should be the hallmark of communication with Board members of any healthcare organization. You should be as objective and informative about the current state of financial affairs. Simultaneously, you can set forth solutions to deal with budgeting issues.
The executive team and CEO should also be clear about the future budgeting decisions that would mitigate cash-flow issues and improve the revenue cycle. However, you also have to take into account the uncertain spike in COVID-19 cases and vaccine data that constantly leave a question mark on your budgeting cycle.
PDV Health Consulting: Take Your Strategic Plan to the Next Level
At PDV Health Consulting, our focus is to determine budget constraints and keep an eye on expenses. We believe that patient care and accessibility will always revolve around perfected revenue cycle management.
For the sake of normal operations during crisis situations and emergencies, revenue cycle management, and positive cash-flow can make all the difference. PDV Health Consulting’s patient access can lend a hand to healthcare organizations and ensure front-end organizational functions are functional at industry standards.
Whether its rework management, processes flows, authorizations, point-of-service collections, or other metrics, we can help you analyze a viable strategic plan that takes into account the intricate details of budgeting.
Our evaluation will help you figure out the elements that would improve your revenue cycle and open new windows of opportunities. Through our informative assessment, you will be able to review departmental preparedness for medical emergencies and offer suggestions to normalize operations.
Conclusion
Healthcare organizations are aware of the lost revenue from cancelled or delayed primary elective procedures. Since revenue continues to plunge, hospitals need to bring the spotlight on expenditures.
Small hospitals, for instance, have to take extra precautions to maintain positive cash-flow despite uncertain economic turmoil. Fortunately, shareholders want to use their creative ingenuity to come up with solutions that work in favor of patients and healthcare organizations.
Undoubtedly, the unconditional support and passion of medical professionals to treat patients despite continuous setbacks and equipment or supplies shortages is applause-worthy. However, CFOs of healthcare organizations have never had to face such rigid financial circumstances. In hindsight, it is high time for healthcare organizations to prepare for a more stable financial future.
Follow us and find out budgeting strategies that can sustain your healthcare organization’s operational activities and help you provide quality patient care at the same time.

